Chinese Journal of Tissue Engineering Research ›› 2016, Vol. 20 ›› Issue (19): 2879-2888.doi: 10.3969/j.issn.2095-4344.2016.19.021
Development of mesenchymal stem cell homing
Deng Rong-rong1, Xie Yi-min2, Xie Lin1
- 1Affiliated Hospital of Integrated Traditional Chinese and Western Medicine, Nanjing University of Chinese Medicine, Nanjing 210000, Jiangsu Province, China
2Nanjing University of Chinese Medicine, Nanjing 210000, Jiangsu Province, China
-
Received:2016-04-02Online:2016-05-06Published:2016-05-06 -
Contact:Xie Lin, M.D., Chief physician, Professor, Affiliated Hospital of Integrated Traditional Chinese and Western Medicine, Nanjing University of Chinese Medicine, Nanjing 210000, Jiangsu Province, China -
About author:Deng Rong-rong, Studying for master’s degree, Affiliated Hospital of Integrated Traditional Chinese and Western Medicine, Nanjing University of Chinese Medicine, Nanjing 210000, Jiangsu Province, China -
Supported by:the Natural Science Foundation of Jiangsu Province, No. BK20151604; the Special Project of Clinical Science and Technology-- Research of New Clinical Diagnosis and Treatment Technology, No. BL2012069
CLC Number:
Cite this article
Deng Rong-rong, Xie Yi-min, Xie Lin. Development of mesenchymal stem cell homing[J]. Chinese Journal of Tissue Engineering Research, 2016, 20(19): 2879-2888.
share this article
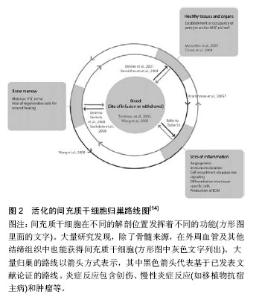
2.1 间充质干细胞的生物学特性 间充质干细胞是一类具有自我更新、高度增殖、免疫调控、造血支持及多向分化潜能的非造血干细胞,最早在骨髓中发现[1],随后在多种组织中发现,如脂肪、脐带沃顿胶、脐血等[2-3]。目前国际公认的人间充质干细胞表型特征为:细胞表面CD73、CD90、CD105等抗原呈阳性,而CD14、CD79a、CD11b、CD19、CD34、CD45、HLA-DR等表达阴性[4]。大多数人类间充质干细胞可以作为中胚层组织如骨骼、脂肪和软骨发育的前体细胞,同时还可以跨越胚层横向分化为各种组织细胞[5-7],如神经细胞和内皮细胞等[8]。 间充质干细胞是一类低免疫原性的成体干细胞,间充质干细胞的低免疫原性与其低表达主要组织相容性复合体MHC-Ⅰ而不表达MHC-Ⅱ、CD40、CD80、CD86有关,同时间充质干细胞对各类免疫细胞均具有免疫调节作用。研究发现间充质干细胞可通过调节T细胞的活化和增殖来抑制免疫反应[9-10]。间充质干细胞对T细胞的调节可通过细胞间直接接触[11-12],亦可在非直接接触下间充质干细胞分泌可溶性因子来发挥作用。内源性间充质干细胞可产生相应的生长因子和细胞因子在组织修复过程中发生作用,如骨形态发生蛋白在骨、肌腱、软骨的修复中发挥作用[13],促血管再生因子可用于缺血性疾病的治疗。基因修饰的干细胞移植是目前临床研究的热点,因此,间充质干细胞的低免疫原性及促进机体修复的特点使其成为备受关注的可用于移植的干细胞之一,而移植的间充质干细胞能否顺利归巢至微环境,是决定间充质干细胞移植的成败之一。 2.2 间充质干细胞的归巢及归巢机制 干细胞归巢是指自体或外源性干细胞在多种因素的作用下,能定向趋向性迁移,越过血管内皮细胞至靶向组织并定植存活的过程,类似人体局部炎症反应后大量白细胞迁移至炎症周围,见图2。2009年Krap等[14]建议将“间充质干细胞归巢”定义为:间充质干细胞在目标组织的脉管系统里被捕获,随后跨越血管内皮细胞迁移至目标组织的过程。间充质干细胞与血管内皮细胞具有相似性,因而易于迁移和植入。干细胞“巢”作为一种特殊的微环境,是干细胞存在的基础,“巢”通过不同信号途径调控着干细胞的行为,使干细胞的生长、更新和分化在生理条件下处于稳定平衡状态。对于归巢机制,尤其是干细胞的动员,目前无法准确的阐述。大部分研究文献基于白细胞迁移、人类干细胞以及转移肿瘤细胞研究干细胞的迁移行为,针对各种细胞表面受体及细胞因子进行探索。"
| [1] Kern S, Eichler H, Stoeve J, et al. Comparative analysis of mesenchymal stem cells from bone marrow, umbilical cord blood, or adipose tissue. Stem Cells. 2006;24(5):1294-1301.[2] Anzalone R, Lo Iacono M, Corrao S, et al. New emerging potentials for human Wharton's jelly mesenchymal stem cells: immunological features and hepatocyte-like differentiative capacity. Stem Cells Dev. 2010;19(4):423-438.[3] Erices A, Conget P, Minguell JJ. Mesenchymal progenitor cells in human umbilical cord blood. Br J Haematol. 2000;109(1):235-242.[4] Sacchetti B, Funari A, Michienzi S, et al. Self-renewing osteoprogenitors in bone marrow sinusoids can organize a hematopoietic microenvironment. Cell. 2007;131(2):324-336.[5] Dietz AB, Padley DJ, Gastineau DA. Infrastructure development for human cell therapy translation. Clin Pharmacol Ther. 2007;82(3):320-324. [6] Karp JM, Leng Teo GS. Mesenchymal stem cell homing: the devil is in the details. Cell Stem Cell. 2009;4(3):206-216.[7] Fekete N, Rojewski MT, Fürst D, et al. GMP-compliant isolation and large-scale expansion of bone marrow-derived MSC. PLoS One. 2012;7(8):e43255.[8] Woodbury D, Schwarz EJ, Prockop DJ, et al. Adult rat and human bone marrow stromal cells differentiate into neurons. J Neurosci Res. 2000;61(4):364-370.[9] Di Nicola M, Carlo-Stella C, Magni M, et al. Human bone marrow stromal cells suppress T-lymphocyte proliferation induced by cellular or nonspecific mitogenic stimuli. Blood. 2002;99(10):3838-3843.[10] Bartholomew A, Sturgeon C, Siatskas M, et al. Mesenchymal stem cells suppress lymphocyte proliferation in vitro and prolong skin graft survival in vivo. Exp Hematol. 2002;30(1):42-48.[11] Krampera M, Glennie S, Dyson J, et al. Bone marrow mesenchymal stem cells inhibit the response of naive and memory antigen-specific T cells to their cognate peptide. Blood. 2003;101(9):3722-3729.[12] Le Blanc K, Tammik L, Sundberg B, et al. Mesenchymal stem cells inhibit and stimulate mixed lymphocyte cultures and mitogenic responses independently of the major histocompatibility complex. Scand J Immunol. 2003;57(1):11-20.[13] Nixon AJ, Goodrich LR, Scimeca MS, et al. Gene therapy in musculoskeletal repair. Ann N Y Acad Sci. 2007;1117:310-327.[14] Karp JM, Leng Teo GS. Mesenchymal stem cell homing: the devil is in the details. Cell Stem Cell. 2009;4(3):206-216.[15] Ringe J, Strassburg S, Neumann K, et al. Towards in situ tissue repair: human mesenchymal stem cells express chemokine receptors CXCR1, CXCR2 and CCR2, and migrate upon stimulation with CXCL8 but not CCL2. J Cell Biochem. 2007;101(1):135-146.[16] Sordi V, Malosio ML, Marchesi F, et al. Bone marrow mesenchymal stem cells express a restricted set of functionally active chemokine receptors capable of promoting migration to pancreatic islets. Blood. 2005; 106(2):419-427.[17] Forte G, Minieri M, Cossa P, et al. Hepatocyte growth factor effects on mesenchymal stem cells: proliferation, migration, and differentiation. Stem Cells. 2006;24(1): 23-33.[18] Cui Y, Madeddu P. The role of chemokines, cytokines and adhesion molecules in stem cell trafficking and homing. Curr Pharm Des. 2011;17(30):3271-3279.[19] Broxmeyer HE. Chemokines in hematopoiesis. Curr Opin Hematol. 2008;15(1):49-58.[20] Moll NM, Ransohoff RM. CXCL12 and CXCR4 in bone marrow physiology. Expert Rev Hematol. 2010;3(3): 315-322.[21] Ghadge SK, Mühlstedt S, Ozcelik C, et al. SDF-1α as a therapeutic stem cell homing factor in myocardial infarction. Pharmacol Ther. 2011;129(1):97-108.[22] Wang Y, Deng Y, Zhou GQ. SDF-1alpha/ CXCR4- mediated migration of systemically transplanted bone marrow stromal cells towards ischemic brain lesion in a rat model. Brain Res. 2008;1195:104-112.[23] Shi M, Li J, Liao L, et al. Regulation of CXCR4 expression in human mesenchymal stem cells by cytokine treatment: role in homing efficiency in NOD/SCID mice. Haematologica. 2007;92(7):897-904.[24] Tang JM, Wang JN, Zhang L,et al. VEGF/SDF-1 promotes cardiac stem cell mobilization and myocardial repair in the infarcted heart. Cardiovasc Res. 2011;91(3):402-411.[25] Bhakta S, Hong P, Koc O. The surface adhesion molecule CXCR4 stimulates mesenchymal stem cell migration to stromal cell-derived factor-1 in vitro but does not decrease apoptosis under serum deprivation. Cardiovasc Revasc Med. 2006;7(1):19-24.[26] Wojakowski W, Tendera M, Micha?owska A, et al. Mobilization of CD34/CXCR4+, CD34/CD117+, c-met+ stem cells, and mononuclear cells expressing early cardiac, muscle, and endothelial markers into peripheral blood in patients with acute myocardial infarction. Circulation. 2004;110(20):3213-3220.[27] Wang Y, Johnsen HE, Mortensen S, et al. Changes in circulating mesenchymal stem cells, stem cell homing factor, and vascular growth factors in patients with acute ST elevation myocardial infarction treated with primary percutaneous coronary intervention. Heart. 2006;92(6):768-774.[28] Schenk S, Mal N, Finan A, et al. Monocyte chemotactic protein-3 is a myocardial mesenchymal stem cell homing factor. Stem Cells. 2007;25(1):245-251.[29] Huang J, Zhang Z, Guo J, et al. Genetic modification of mesenchymal stem cells overexpressing CCR1 increases cell viability, migration, engraftment, and capillary density in the injured myocardium. Circ Res. 2010;106(11):1753-1762.[30] Guo J, Zhang H, Xiao J, et al. Monocyte chemotactic protein-1 promotes the myocardial homing of mesenchymal stem cells in dilated cardiomyopathy. Int J Mol Sci. 2013;14(4):8164-8178.[31] Que W, Chen J. Knockdown of c-Met inhibits cell proliferation and invasion and increases chemosensitivity to doxorubicin in human multiple myeloma U266 cells in vitro. Mol Med Rep. 2011; 4(2):343-349.[32] Molnarfi N, Benkhoucha M, Funakoshi H, et al. Hepatocyte growth factor: A regulator of inflammation and autoimmunity. Autoimmun Rev. 2015;14(4):293-303.[33] Baek SJ, Kang SK, Ra JC. In vitro migration capacity of human adipose tissue-derived mesenchymal stem cells reflects their expression of receptors for chemokines and growth factors. Exp Mol Med. 2011; 43(10):596-603.[34] Aenlle KK, Curtis KM, Roos BA, et al. Hepatocyte growth factor and p38 promote osteogenic differentiation of human mesenchymal stem cells. Mol Endocrinol. 2014;28(5):722-730.[35] Kucia M, Zhang YP, Reca R, et al. Cells enriched in markers of neural tissue-committed stem cells reside in the bone marrow and are mobilized into the peripheral blood following stroke. Leukemia. 2006; 20(1):18-28.[36] Trapp T, Kögler G, El-Khattouti A, et al. Hepatocyte growth factor/c-MET axis-mediated tropism of cord blood-derived unrestricted somatic stem cells for neuronal injury. J Biol Chem. 2008;283(47): 32244-32253.[37] 黄小兵,李靖,梁平,等.龟板含药血清对骨髓间充质干细胞 c-met 表达及迁移的影响[J].中国中西医结合消化杂志, 2013,21(11): 569-571.[38] Liu J, Pan G, Liang T, et al. HGF/c-Met signaling mediated mesenchymal stem cell-induced liver recovery in intestinal ischemia reperfusion model. Int J Med Sci. 2014;11(6):626-633.[39] Liu X, Shen W, Yang Y, et al. Therapeutic implications of mesenchymal stem cells transfected with hepatocyte growth factor transplanted in rat kidney with unilateral ureteral obstruction. J Pediatr Surg. 2011;46(3):537-545.[40] Brooke G, Tong H, Levesque JP, et al. Molecular trafficking mechanisms of multipotent mesenchymal stem cells derived from human bone marrow and placenta. Stem Cells Dev. 2008;17(5):929-940.[41] Steingen C, Brenig F, Baumgartner L, et al. Characterization of key mechanisms in transmigration and invasion of mesenchymal stem cells. J Mol Cell Cardiol. 2008;44(6):1072-1084.[42] Segers VF, Van Riet I, Andries LJ, et al. Mesenchymal stem cell adhesion to cardiac microvascular endothelium: activators and mechanisms. Am J Physiol Heart Circ Physiol. 2006;290(4):H1370-1377.[43] 陆紫媛. TNF-α通过ERK/JNK-NF-κB信号通路刺激骨髓间充质干细胞表达VCAM-1[D].广州:南方医科大学, 2014.[44] 吕浩敏,王爱玲,万俊. 黏附分子在骨髓间充质干细胞的表达及向心肌梗死区归巢的作用[J]. 安徽医科大学学报, 2012, 47(4): 415-418.[45] Ip JE, Wu Y, Huang J, et al. Mesenchymal stem cells use integrin beta1 not CXC chemokine receptor 4 for myocardial migration and engraftment. Mol Biol Cell. 2007;18(8):2873-2882.[46] Ruoslahti E. Fibronectin in cell adhesion and invasion. Cancer Metastasis Rev. 1984;3(1):43-51.[47] Discher DE, Janmey P, Wang YL. Tissue cells feel and respond to the stiffness of their substrate. Science. 2005;310(5751):1139-1143.[48] Oakes PW, Patel DC, Morin NA, et al. Neutrophil morphology and migration are affected by substrate elasticity. Blood. 2009;114(7):1387-1395.[49] O'Connor RS, Hao X, Shen K, et al. Substrate rigidity regulates human T cell activation and proliferation. J Immunol. 2012;189(3):1330-1339.[50] Engler AJ, Sen S, Sweeney HL, et al. Matrix elasticity directs stem cell lineage specification. Cell. 2006; 126(4):677-689.[51] Zhang YH, Zhao CQ, Jiang LS, et al. Substrate stiffness regulates apoptosis and the mRNA expression of extracellular matrix regulatory genes in the rat annular cells. Matrix Biol. 2011;30(2):135-144.[52] Schmidt A, Ladage D, Schinköthe T, et al. Basic fibroblast growth factor controls migration in human mesenchymal stem cells. Stem Cells. 2006;24(7): 1750-1758.[53] Williams CK, Segarra M, Sierra Mde L, et al. Regulation of CXCR4 by the Notch ligand delta-like 4 in endothelial cells. Cancer Res. 2008;68(6): 1889-1895.[54] Leong KG, Hu X, Li L, et al. Activated Notch4 inhibits angiogenesis: role of beta 1-integrin activation. Mol Cell Biol. 2002;22(8):2830-2841.[55] Wu Y, Zhao RC. The role of chemokines in mesenchymal stem cell homing to myocardium. Stem Cell Rev. 2012;8(1):243-250.[56] Fatimah SS, Tan GC, Chua K, et al. Stemness and angiogenic gene expression changes of serial-passage human amnion mesenchymal cells. Microvasc Res. 2013;86:21-29.[57] 靳建亮. 原代和反复传代的骨髓间充质干细胞移植在治疗急性心肌梗死作用中的比较研究[D].南京:南京医科大学, 2009.[58] Chen T, Zhang P, Fan W, et al. Co-transplantation with mesenchymal stem cells expressing a SDF-1/HOXB4 fusion protein markedly improves hematopoietic stem cell engraftment and hematogenesis in irradiated mice. Am J Transl Res. 2014;6(6):691-702.[59] 孙瑞婷. HGF 基因修饰的间充质干细胞移植干预放射性肠损的实验研究[D]. 北京:北京工业大学, 2014.[60] 何秀华,李东良,江军,等.移植途径对大鼠骨髓间充质干细胞归巢及肝功能恢复的影响[J]. 中华细胞与干细胞杂志:电子版, 2011, 1(1): 57-62.[61] Chamberlain J, Yamagami T, Colletti E, et al. Efficient generation of human hepatocytes by the intrahepatic delivery of clonal human mesenchymal stem cells in fetal sheep. Hepatology. 2007;46(6):1935-1945.[62] Yang Y, Rossi FM, Putnins EE. Ex vivo expansion of rat bone marrow mesenchymal stromal cells on microcarrier beads in spin culture. Biomaterials. 2007; 28(20):3110-3120.[63] 沈运丽. 外加磁场引导下骨髓间充质干细胞靶向修复缺血心肌的实验研究[D].上海:复旦大学, 2013.[64] di Bonzo LV, Ferrero I, Cravanzola C, et al. Human mesenchymal stem cells as a two-edged sword in hepatic regenerative medicine: engraftment and hepatocyte differentiation versus profibrogenic potential. Gut. 2008 Feb;57(2):223-231.[65] 杨屹,张明宇,屈波,等.射频肝损伤血清诱导兔骨髓干细胞向肝细胞样分化[J].第四军医大学学报, 2008, 29(12): 1100-1103.[66] Mohsin S, Shams S, Ali Nasir G, et al. Enhanced hepatic differentiation of mesenchymal stem cells after pretreatment with injured liver tissue. Differentiation. 2011;81(1):42-48.[67] 王莹,赵文静,叶冬霞,等.急性肝衰竭大鼠血清诱导骨髓间充质干细胞表达甲胎蛋白和白蛋白[J].中国组织工程研究与临床康复,2010,14(45): 8369-8372.[68] Shi XL, Gu JY, Zhang Y, et al. Protective effects of ACLF sera on metabolic functions and proliferation of hepatocytes co-cultured with bone marrow MSCs in vitro.World J Gastroenterol. 2011;17(19):2397-2406.[69] Omori Y, Honmou O, Harada K, et al. Optimization of a therapeutic protocol for intravenous injection of human mesenchymal stem cells after cerebral ischemia in adult rats. Brain Res. 2008;1236:30-38.[70] Sotiropoulou PA, Perez SA, Salagianni M, et al. Characterization of the optimal culture conditions for clinical scale production of human mesenchymal stem cells. Stem Cells. 2006;24(2):462-471.[71] Lee WY, Park KJ, Cho YB, et al. Autologous adipose tissue-derived stem cells treatment demonstrated favorable and sustainable therapeutic effect for Crohn's fistula. Stem Cells. 2013;31(11):2575-2581.[72] Hare JM, Fishman JE, Gerstenblith G, et al. Comparison of allogeneic vs autologous bone marrow–derived mesenchymal stem cells delivered by transendocardial injection in patients with ischemic cardiomyopathy: the POSEIDON randomized trial. JAMA. 2012;308(22):2369-2379.[73] Khubutiya MS, Vagabov AV, Temnov AA, et al. Paracrine mechanisms of proliferative, anti-apoptotic and anti-inflammatory effects of mesenchymal stromal cells in models of acute organ injury. Cytotherapy. 2014;16(5):579-585.[74] Stoicov C, Li H, Liu JH, et al. Mesenchymal stem cells utilize CXCR4-SDF-1 signaling for acute, but not chronic, trafficking to gastric mucosal inflammation. Dig Dis Sci. 2013;58(9):2466-2477. |
| [1] | Pu Rui, Chen Ziyang, Yuan Lingyan. Characteristics and effects of exosomes from different cell sources in cardioprotection [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(在线): 1-. |
| [2] | Lin Qingfan, Xie Yixin, Chen Wanqing, Ye Zhenzhong, Chen Youfang. Human placenta-derived mesenchymal stem cell conditioned medium can upregulate BeWo cell viability and zonula occludens expression under hypoxia [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(在线): 4970-4975. |
| [3] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [4] | Hou Jingying, Yu Menglei, Guo Tianzhu, Long Huibao, Wu Hao. Hypoxia preconditioning promotes bone marrow mesenchymal stem cells survival and vascularization through the activation of HIF-1α/MALAT1/VEGFA pathway [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 985-990. |
| [5] | Shi Yangyang, Qin Yingfei, Wu Fuling, He Xiao, Zhang Xuejing. Pretreatment of placental mesenchymal stem cells to prevent bronchiolitis in mice [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 991-995. |
| [6] | Liang Xueqi, Guo Lijiao, Chen Hejie, Wu Jie, Sun Yaqi, Xing Zhikun, Zou Hailiang, Chen Xueling, Wu Xiangwei. Alveolar echinococcosis protoscolices inhibits the differentiation of bone marrow mesenchymal stem cells into fibroblasts [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 996-1001. |
| [7] | Fan Quanbao, Luo Huina, Wang Bingyun, Chen Shengfeng, Cui Lianxu, Jiang Wenkang, Zhao Mingming, Wang Jingjing, Luo Dongzhang, Chen Zhisheng, Bai Yinshan, Liu Canying, Zhang Hui. Biological characteristics of canine adipose-derived mesenchymal stem cells cultured in hypoxia [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1002-1007. |
| [8] | Geng Yao, Yin Zhiliang, Li Xingping, Xiao Dongqin, Hou Weiguang. Role of hsa-miRNA-223-3p in regulating osteogenic differentiation of human bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1008-1013. |
| [9] | Lun Zhigang, Jin Jing, Wang Tianyan, Li Aimin. Effect of peroxiredoxin 6 on proliferation and differentiation of bone marrow mesenchymal stem cells into neural lineage in vitro [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1014-1018. |
| [10] | Zhu Xuefen, Huang Cheng, Ding Jian, Dai Yongping, Liu Yuanbing, Le Lixiang, Wang Liangliang, Yang Jiandong. Mechanism of bone marrow mesenchymal stem cells differentiation into functional neurons induced by glial cell line derived neurotrophic factor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1019-1025. |
| [11] | Duan Liyun, Cao Xiaocang. Human placenta mesenchymal stem cells-derived extracellular vesicles regulate collagen deposition in intestinal mucosa of mice with colitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1026-1031. |
| [12] | Pei Lili, Sun Guicai, Wang Di. Salvianolic acid B inhibits oxidative damage of bone marrow mesenchymal stem cells and promotes differentiation into cardiomyocytes [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1032-1036. |
| [13] | Wang Xianyao, Guan Yalin, Liu Zhongshan. Strategies for improving the therapeutic efficacy of mesenchymal stem cells in the treatment of nonhealing wounds [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1081-1087. |
| [14] | Wang Shiqi, Zhang Jinsheng. Effects of Chinese medicine on proliferation, differentiation and aging of bone marrow mesenchymal stem cells regulating ischemia-hypoxia microenvironment [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1129-1134. |
| [15] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||